Authors: CM Emerson MS41, MN Greco MS41, TJ O’Neil MS41, CE White MS41; SM O’Neil, MD, FACS2,3
1Campbell University School of Osteopathic Medicine, 2Martinsville Surgical Associates, 3SOVAH Health
ABSTRACT:
Introduction
Dog bite injuries are a common presenting complaint to emergency departments across the country. However, there is a current lack of literature regarding the evaluation and management of non-fatal dog bite injuries. These injuries can therefore present challenges to emergency medicine providers due to lack of clear guidance on their evaluation and management. The majority of dog bites occur to the upper extremities and are superficial injuries, however more severe injuries and complications can occur. The potential for neurovascular injuries should not be overlooked. Physical examination findings can be helpful, but are at times unreliable. Imaging studies are commonly required to characterize the full extent of injury.
Case
We present the case detailing the management of a 40-year-old male that presented to the emergency department with five separate puncture wounds after sustaining a dog bite injury to his left upper extremity.
Conclusion
This case report highlights the emergent evaluation and management of dog bite injuries and the importance of ultrasound in the early identification of complications, such as vascular trauma, that can result from these injuries.
INTRODUCTION:
- Epidemiology & Demographics:
There is a current lack of literature regarding the evaluation and management of dog bite injuries presenting to emergency departments (EDs), despite dog bites being a common presenting injury. Several studies have attempted to assess the demographics and epidemiology of these injuries presenting to emergency departments [1-6]. One analysis from the 1990s showed that approximately 333,687 dog bite injuries were treated annually in emergency departments [1]. More recent studies have shown that these cases have continued to increase, reporting numbers even up to 450,000 annually [2, 3].
In addition to the psychological burden dog bite injuries may cause patients, these injuries pose a significant financial burden, especially in the cases of injuries requiring IV antibiotics, hospital admission, or surgical intervention [7,8]. The aggregate cost of dog bite related hospitalizations is $53.9 million annually [7]. According to the Health Care Cost Institute, in 2016 the average price of an ED visit in the US was $1,917.20 [9,10]. The cost of a dog bite related injury significantly increased if a hospital admission was required, with average costs being greater than $18,200 [7,9-10], and even more if a surgical admission was required [9-10].
The demographics of patients sustaining dog bite injuries have been analyzed by multiple retrospective studies. These studies have shown that the majority of adult patients presenting to the ED from sustained dog bite injuries were usually male [3,5,8,11] and most commonly had injuries to the hands and upper extremity [3-7,11]. While dog bite injuries occur across all age groups, admissions were more common for older and younger patients [3], possibly due to a more frequent need for aggressive medical care. Factors contributing to a higher likelihood of admission in adult patients included older age, comorbidities, increased number of prior presentations, presence of infection, or complicated injuries [3-4,8,12]. Certain factors also increased the risk of infection, including crush injuries or puncture wounds, bites in extremities (with underlying venous and/or lymphatic compromise), injuries to the upper or lower extremity that were delayed more than 6-12 hours on presentation, or concurrent diabetes mellitus [13].
- Examination of dog bite injuries for complications:
While dog bite injuries in children have been described in detail, dog bite injuries in adults are less well studied [2,4,13]. The majority of dog bites in adult patients are usually minor, most commonly resulting in superficial injuries [4,6]. However, there is potential for a spectrum of more severe injuries and complications that cannot be overlooked. These include crush injuries, deep puncture wounds, tissue avulsions, abrasions, fractures, dislocations, lacerations, or combinations of these [4-6,8,11-12]. Neurovascular injuries, tendon dysfunction, amputations, and death have also been reported in the literature [5-6,11,14].
Infections are a common complication associated with dog bite injuries. Infections occurred most often in patients with injuries to the hands and were associated with a greater need for surgical treatment [4-5,12]. Lower rates of infection were seen in patients prescribed prophylactic antibiotics with initial injury presentation [4,12,15]. However, failure to implement prophylactic antibiotics was not always associated with increased risk of subsequent ED presentations related to infections, suggesting it is unclear as to whether every patient presenting with dog bite injuries should receive antibiotic treatment [4,16,17].
Vascular injuries are a rare, but serious complication of dog bite injuries to the extremities that indicate the need for surgical exploration. A high index of suspicion is required in the evaluation of adult patients presenting with dog bite injuries as the presence of vascular trauma is unpredictable [5]. Several studies demonstrated physical findings that may indicate underlying vascular injury, which include hard and soft signs such as extremity pulse abnormalities, absent palpable distal pulse with Doppler ultrasound, or neurological deficits [11,14,18].
Imaging studies are also commonly required to characterize the extent of injury. Radiography is commonly the first imaging technique for animal bite injuries [19]. One of the most common indications for further imaging of these injuries is to exclude infection of the wound. However, in cases where vascular injury is suspected, point-of-care ultrasonography or duplex ultrasonography/duplex study, CT angiography (CTA), magnetic resonance imaging (MRI), contrast angiography, can be used to assess surrounding vessels for damage and determine the need for surgical intervention [11,19].
- Current guidelines on evaluation and management:
Despite how common dog bites are as a presenting cause of injury to the ED, there are no clear guidelines for evaluation or intervention for these injuries. It appears there is ongoing controversy regarding use of prophylactic antibiotics and primary versus secondary wound closure [6]. The current standard of care for emergent evaluation of a non-life-threatening dog bite involves local wound irrigation, antibiotic treatment, consideration for rabies prophylaxis, and primary wound closure to avoid infections [2,6,12-13]. These practices are consistent with the key, but general, recommendations listed by the American Academy of Family Physicians (AAFP) for the management of dog and cat bites. Surgical intervention is often also required due to the potential for neurovascular trauma. However, there are no consistent clinical criteria indicating when surgical intervention is needed to address injuries or complications sustained from dog bites to the extremities [5,11,14].
- Purpose:
This work presents the case of an adult patient that was seen in multiple EDs after sustaining a dog bite to the left upper extremity and evaluates current emergent management of dog bite injuries presenting to the emergency department. This report highlights the importance of prompt recognition and management of vascular injuries following dog bites to optimize patient outcomes and ultimately avoid further complications.
CASE DESCRIPTION:
A 40-year-old male with no history of chronic illness presented to the emergency department with five separate puncture wounds after sustaining a dog bite injury to his left upper extremity. Lacerations were irrigated, three were sutured, and the patient was discharged on a single-antibiotic regimen of Augmentin.
The patient presented to a separate emergency department four days later with swelling, pain, and decreased radial pulse in the left upper extremity. Physical examination was positive for fever, chills, rigor, and marked erythema from the distal ¾ of the anterior medial aspect of the left upper extremity to the proximal ¼ of the forearm. Neuromuscular testing demonstrated function was intact in the left upper extremity. The patient was diagnosed with acute cellulitis of the left upper extremity secondary to an infected dog bite and admitted for inpatient intravenous (IV) antibiotics. The patient was started on IV Levofloxacin 150 mL and IV Clindamycin 37.5 mL.
After two days on inpatient service, the left radial pulse was still weak, prompting further investigation via duplex ultrasonography. The visualized vessels of the left upper extremity appeared widely patent, however, the proximal brachial artery was not visualized in the region of the trauma. Flow patterns of the mid-upper arm and onward were post-obstructive with normal velocities, suggestive of collateral blood supply. There was a significant velocity drop to 30 cm/sec (normal: 40-90 cm/sec) between the mid- and distal-brachial artery, suggesting hemodynamically significant stenosis in the region of the mid-brachial artery (Figure 1).
Figure 1
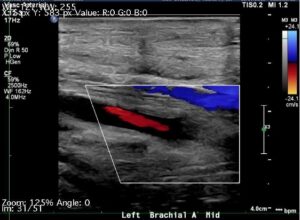
Figure 1. Right upper extremity arterial duplex with minimal to absent flow in the mid-brachial artery and occlusion of the vessel.
Absent left brachial artery flow and significant velocity drop on arterial duplex study prompted the need for further work up with CTA. CTA revealed a 15-20 mm segment of the left mid-brachial artery that showed non-filling, which confirmed complete occlusion at the mid-left brachial artery and revealed a side branch of collateral circulation proximal to the occluded segment (Figure 2), as initially suspected by the arterial duplex study. There was no evidence of embolus, aneurysm, surrounding hematoma, or compartment syndrome.
Figure 2
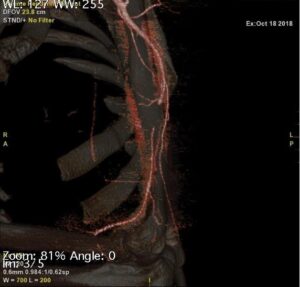
Figure 2. Computed tomography angiography of left upper extremity with reconstruction visualizing complete occlusion of brachial artery and collateral branch artery keeping the lower arm viable.
The patient was referred to surgery. The patient was sedated using general anesthesia with laryngeal mask airway for a planned thrombectomy, excision of segmental left brachial artery, and placement of reversed saphenous vein interposition graft. Pre-operative exams revealed no palpable pulses of the left radial or ulnar arteries. Upon dissection, the brachial artery showed redness, induration, and fibrosis. A 3-French Fogarty was inserted and inflated. Flow resumed but stopped after 5 seconds. The arteriotomy was extended proximally and a large thrombus was identified. The posterior wall of the left brachial artery was found to be completely torn with thrombosis and occlusion of the area. A 2-inch saphenous vein graft was harvested from the right lower extremity and was surgically anastomosed to the healthy brachial artery proximally and distally to the occlusion and tear. Blood flow resumed with palpable left radial and ulnar pulses on post-intervention exam. The patient had complete resolution of the injury without further need for intervention.
Discussion:
Dog bite injuries are a common presenting complaint to emergency departments across the US. There is a current lack of literature regarding the evaluation and management of adult dog bite injuries presenting to emergency departments, despite dog bites being a common presenting injury. It is possible this is due to the inconsitency of injury documentation and ICD coding in hospital systems across the United States, leading to an understatement of the need for clear guidance on emergency physician management of these injuries.
The AAFP lists key recommendations for management of animal bites. However, they are general and non-specific to dog bite injuries presenting in an ED setting. Likewise, criteria for surgical intervention for possible neurovascular complications of dog bite injuries is also not consistently indicated in the literature. Regarding the AAFP’s recommendations, pre-exposure and post-exposure rabies prophylaxis had the highest level of evidence-based support, and proper wound care was considered essential to preventing secondary infection [13]. Wound closure had a lower level of evidence, with recommendations based on inconsistent or limited quality patient-oriented evidence [13]. The current standard of care for emergency department management is consistent with the AAFP recommendations and involves local wound irrigation, antibiotic treatment, consideration for rabies prophylaxis, and primary wound closure to avoid infections [2,6,12-13]. Amoxicillin and Clavulanate are the most common prophylactic antibiotics [4,6,13].
The demographics of patients sustaining dog bite injuries have been analyzed by multiple retrospective studies [1-6]. Aligning with the case, the majority of adult patients presenting to the ED after sustaining a dog bite are male with injuries to the upper extremity. On average, the cost of dog bite related injuries requiring hospital admission is greater than $18,200, and $41,701.60 if surgical management is required [7,9-10]. The cost of care for our patient was likely even higher, as the patient was not admitted for further workup and management of his injury until his second ED presentation and his injury ultimately required surgical intervention.
Despite the fact most dog bites in adult patients only result in superficial injuries [4,6], the possibility of severe underlying injuries and complications cannot be overlooked. Infections and neurovascular injuries are important considerations for every patient presenting to the emergency department with dog bite injuries [4-6,11-12,14]. The presence of vascular trauma is unpredictable and multiple retrospective studies have failed to identify reliable associations between presenting factors and necessity for admission [3,5]. Several studies demonstrated physical findings that may indicate underlying vascular injury, which include hard and soft signs such as extremity pulse abnormalities, absent palpable distal pulse with doppler ultrasound, and neurological deficits [11,14,18]. However, the sample sizes were quite small for extrapolation to the general population. Therefore, while physical exam findings may indicate underlying vascular injury, they are unreliable overall as seen in this case. Objective measures like imaging studies (such as point-of-care ultrasound or duplex ultrasonography), can more reliably be used to assess vascular injury and determine the need for further surgical intervention. CTA is also a valuable option for assessing damage to underlying vessels. One retrospective study showed CTA performed in patients presenting with abnormal pulses after dog bite injury was consistently diagnostic of vascular injury [11]. However, if physical signs of neurovascular compromise are present, these are strong indicators that surgical intervention is urgently needed.
This work presented the case of an adult patient that was seen in multiple EDs after sustaining a dog bite to the left upper extremity that resulted in vascular complications. Given the intraoperative findings, the occlusion in this case was likely due to thrombosis following a vessel wall tear from the dog bite. The patient’s left upper extremity was saved from ischemia due to a smaller collateral brachial artery branch supplying the arterial system distal to the injury.
This work analyzed the current guidelines for dog bite injuries presenting to the emergency department and the need for clear guidance in their emergent management. This case also highlights the importance of utilizing imaging in the initial emergency department evaluation for prompt recognition and management of vascular injuries following dog bites injuries. Had there been a higher index of suspicion for the possibility of vascular trauma following the dog bite injury sustained by our patient, duplex ultrasonography could have been used on the patient’s first presentation, allowing for earlier identification of the vascular injury in the course of this patient’s care. Missing this finding in the first ED visit could have proved more detrimental if not for the collateral artery that was present. These key findings in our case are discussed to help optimize future patient outcomes and ultimately avoid further complications.
Conclusion:
Most injuries resulting from dog bites to the extremities are superficial and are often adequately addressed with local wound irrigation, antibiotics, and primary closure. However, the potential for more serious complications from dog bite injuries cannot be overlooked. A high index of suspicion for the presence of neurovascular injuries is required during the initial evaluation, as the presence of vascular trauma is unpredictable. An adequate physical examination looking for signs of neurovascular compromise is vital in the first steps of working up these patients. However, findings on physical exam have been shown to not consistently be reproducible, therefore additional imaging such as doppler ultrasound or CTA may be required to fully detect the presence of underlying vascular injuries.
References
1) Weiss HB, Friedman DI, Coben JH. Incidence of dog bite injuries treated in emergency departments. JAMA. 1998;279(1):51-53. doi:10.1001/jama.279.1.51
2) Ramgopal S, Macy ML. US estimates for dog bite injuries presenting to emergency departments. Public Health. 2021;196:1-3. doi:10.1016/j.puhe.2021.04.028
3) Loder RT. The demographics of dog bites in the United States. Heliyon. 2019;5(3):e01360. Published 2019 Mar 20. doi:10.1016/j.heliyon.2019.e01360
4) Pfortmueller CA, Efeoglou A, Furrer H, Exadaktylos AK. Dog bite injuries: primary and secondary emergency department presentations–a retrospective cohort study. ScientificWorldJournal. 2013;2013:393176. Published 2013 Sep 24. doi:10.1155/2013/393176
5) Benfield R, Plurad DS, Lam L, et al. The epidemiology of dog attacks in an urban environment and the risk of vascular injury. Am Surg. 2010;76(2):203-205.
6) Morzycki A, Simpson A, Williams J. Dog bites in the emergency department: a descriptive analysis. CJEM. 2019;21(1):63-70. doi:10.1017/cem.2018.2.
7) Holmquist L, Elixhauser A. Emergency Department Visits and Inpatient Stays Involving Dog Bites, 2008. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. Rockville (MD): Agency for Healthcare Research and Quality (US); November 2010.
8) Rhea S, Weber DJ, Poole C, Cairns C. Risk factors for hospitalization after dog bite injury: a case-cohort study of emergency department visits. Acad Emerg Med. 2014;21(2):196-203. doi:10.1111/acem.12312
9) Health Care Cost Institute; 2018. 2016-HCCUR-Appendix-Tables-1.23.18-c. http://www.healthcostinstitute.org/report/2016-health-care-cost-utilization-report/
10) Frost A., Hargraves J., Rodriguez S., Brennan N. Health Care Cost Institute; 2018. 2016 Health Care Cost and Utilization Report.
11) Akingba AG, Robinson EA, Jester AL, et al. Management of vascular trauma from dog bites. J Vasc Surg. 2013;58(5):1346-1352. doi:10.1016/j.jvs.2013.05.101
12) Philipsen TE, Molderez C, Gys T. Cat and dog bites. What to do? Guidelines for the treatment of cat and dog bites in humans. Acta Chir Belg. 2006;106(6):692-695. doi:10.1080/00015458.2006.11679983
13) Ellis R, Ellis C. Dog and cat bites. Am Fam Physician. 2014;90(4):239-243.
14) Alluri RK, Pannell W, Heckmann N, Sivasundaram L, Stevanovic M, Ghiassi A. Predictive Factors of Neurovascular and Tendon Injuries Following Dog Bites to the Upper Extremity. Hand (N Y). 2016;11(4):469-474. doi:10.1177/1558944715620794
15) Cummings P. Antibiotics to prevent infection in patients with dog bite wounds: a meta-analysis of randomized trials. Ann Emerg Med. 1994;23(3):535-540. doi:10.1016/s0196-0644(94)70073-7
16) Rothe M, Rudy T, Stanković P. Die Therapie von Bissverletzungen der Hand und des Handgelenkes – Ist eine Antibiotika-Prophylaxe in jedem Fall notwendig?1 [Treatment of bites to the hand and wrist–is the primary antibiotic prophylaxis necessary?]. Handchir Mikrochir Plast Chir. 2002;34(1):22-29. doi:10.1055/s-2002-22103
17) Medeiros I, Saconato H. Antibiotic prophylaxis for mammalian bites. Cochrane Database Syst Rev. 2001;(2):CD001738. doi:10.1002/14651858.CD001738
18) Cawley OV, Walsh AS, Asghar I, Desmarowitz HU, Antoniou GA. Arterial Injury in the Upper Limb Resulting from Dog Bite. Ann Vasc Surg. 2018;49:314.e5-314.e10. doi:10.1016/j.avsg.2017.11.053
19) Young PM, Bancroft LW, Peterson JJ, Roberts CC, Liu PT, Zaleski CG. Imaging spectrum of bites, stings, and their complications: pictorial review. AJR Am J Roentgenol. 2009;193(3 Suppl):S31-S45. doi:10.2214/AJR.07.7123
