Parham Salehi Saee, MS3; Nathan C Ellis, MD; Dhimitri A Nikolla, DO; Melody Milliron, DO
Affiliations:
1Lake Erie College of Osteopathic Medicine, Erie, PA.
2Department of Emergency Medicine, Saint Vincent Hospital, Allegheny Health Network, Erie, PA.
Corresponding Author:
Dhimitri A. Nikolla, DO
Department of Emergency Medicine
Saint Vincent Hospital
Allegheny Health Network
232 West 25th Street
Erie, PA, 16544
Email: dhimitri.nikolla@med.lecom.edu
Twitter Handle: @DhimitriNikolla
MANUSCRIPT
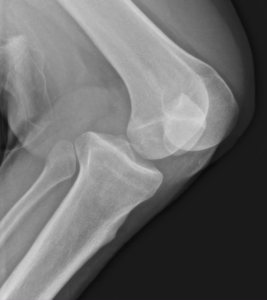
A 23-year-old male presented to the emergency department (ED) with acute pain and deformity of the left knee after falling off his skateboard. Examination revealed the knee bent 90 degrees with posterior displacement of the proximal tibia. Motor, sensory, and pulses intact in the left foot. Lateral radiograph revealed a posterior dislocation of left knee (image). Closed reduction and splinting were performed in the ED with procedural sedation. Computed tomography angiography (CTA) revealed no evidence of acute popliteal arterial vascular injury. The patient was admitted and magnetic resonance imaging revealed ligamentous injuries to the anterior, posterior, and medial collateral ligaments (ACL, PCL, MCL). He underwent open repair of the MCL the next day with plans for delayed treatment of the ACL and PCL injuries after physical therapy to improve strength and knee range of motion.
Posterior knee dislocations are high energy injuries usually caused by a direct impact on the proximal tibia resulting in posterior dislocation with respect to the distal femur.1 They usually present with severe pain, swelling, instability and limited range of motion of the knee. Spontaneous reduction prior to ED arrival may allow the dislocation to go unrecognized despite imaging and result in delayed diagnosis.2 Up to 32% of knee dislocations are complicated by vascular injury; most commonly popliteal artery injury.3, 4 Nevertheless, selective CTA based on history and physical examination is more commonly recommended than routine angiography.4, 5